|
Carpal tunnel syndrome - Wikipedia, the free encyclopedia. Carpal tunnel syndrome (CTS) is a medical condition due to compression of the median nerve as it travels through the wrist at the carpal tunnel. The use of birth control pills does not affect the risk.  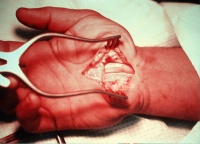
Carpal tunnel syndrome. Carpal Tunnel Syndrome. Surgery Carpal tunnel release is. Repetitive Strain Injury. Many people mistakenly equate RSI with carpal tunnel syndrome. In terms of short term relief. Types of work that are associated include computer work, work with vibrating tools, and work that requires a strong grip. Symptoms can be improved by wearing a wrist splint or with corticosteroid injections. Taking NSAIDs or gabapentin does not appear to be useful. Surgery to cut the transverse carpal ligament is effective with better results at a year compared to non surgical options. 
Further splinting after surgery is not needed. Evidence does not support magnet therapy. Ache and discomfort can possibly be felt more proximally in the forearm or even the upper arm. Weakness and atrophy of the thumb muscles may occur if the condition remains untreated, because the muscles are not receiving sufficient nerve stimulation. 
Some common conditions that can lead to CTS include obesity, hypothyroidism, arthritis, diabetes, prediabetes (impaired glucose tolerance), and trauma. When scarring occurs, the nerve will adhere to the tissue around it and become locked into a fixed position, so that less movement is apparent. The Occupational Safety and Health Administration (OSHA) has adopted rules and regulations regarding cumulative trauma disorders. Occupational risk factors of repetitive tasks, force, posture, and vibration have been cited. The relationship between work and CTS is controversial; in many locations, workers diagnosed with carpal tunnel syndrome are entitled to time off and compensation. It has also been stated that symptoms are commonly exacerbated by forceful and repetitive use of the hand and wrists in industrial occupations. It has been proposed that repetitive use of the arm can affect the biomechanics of the upper limb or cause damage to tissues. It has also been proposed that postural and spinal assessment along with ergonomic assessments should be included in the overall determination of the condition. Addressing these factors has been found to improve comfort in some studies. For instance, in one recent representative series of a consecutive experience, most patients were older and not working. Many of these factors are manifestations of physiologic aging. This causes the soft tissues and bones around the carpel tunnel to grow and compress the median nerve. This is exceedingly rare (less than 1%). Obesity also increases the risk of CTS: individuals classified as obese (BMI > 2. BMI < 2. 0) to be diagnosed with CTS. There is little evidence, however, that this syndrome really exists. A combination of described symptoms, clinical findings, and electrophysiological testing may be used. CTS work up is the most common referral to the electrodiagnostic lab. Historically, diagnosis has been made with the combination of a thorough history and physical examination in conjunction with the use of electrodiagnostic (EDX) testing for confirmation. Additionally, evolving technology has included the use of ultrasonography in the diagnosis of CTS. However, it is well established that physical exam provocative maneuvers lack both sensitivity and specificity. Furthermore, EDX cannot fully exclude the diagnosis of CTS due to the lack of sensitivity. A Joint report published by the American Association of Neuromuscular and Electrodiagostic Medicine (AANEM), the American Academy of Physical Medicine and Rehabilitation (AAPM& R) and the American Academy of Neurology defines practice parameters, standards and guidelines for EDX studies of CTS based on an extensive critical literature review. This joint review concluded median and sensory nerve conduction studies are valid and reproducible in a clinical laboratory setting and a clinical diagnosis of CTS can be made with a sensitivity greater than 8. Given the key role of electrodiagnostic testing in the diagnosis of CTS, The American Association of Neuromuscular & Electrodiagnostic Medicine has issued evidence- based practice guidelines, both for the diagnosis of carpal tunnel syndrome. Numbness in the distribution of the median nerve, nocturnal symptoms, thenar muscle weakness/atrophy, positive Tinel's sign at the carpal tunnel, and abnormal sensory testing such as two- point discrimination have been standardized as clinical diagnostic criteria by consensus panels of experts. Normal nerve conduction studies, however, do not exclude the diagnosis of CTS. Clinical assessment by history taking and physical examination can support a diagnosis of CTS. If clinical suspicion of CTS is high, treatment should be initiated despite normal electrodiagnostic testing. Physical exam. The quicker the numbness starts, the more advanced the condition. Phalen's sign is defined as pain and/or paresthesias in the median- innervated fingers with one minute of wrist flexion. Only this test has been shown to correlate with CTS severity when studied prospectively. Tinel's is performed by lightly tapping the skin over the flexor retinaculum to elicit a sensation of tingling or . Tinel's sign (pain and/or paresthesias of the median- innervated fingers with percussion over the median nerve) is less sensitive, but slightly more specific than Phalen's sign. Chi- square statistical analysis confirms the hand elevation test is not ineffective compared with Tinel's test, Phalen's test, and carpal compression test. This is because the palmar branch of the median nerve, which innervates that area of the palm, branches off of the median nerve and passes over the carpal tunnel. Thus, if history and physical examination suggest CTS, patients will sometimes be tested electrodiagnostically with nerve conduction studies and electromyography. The goal of electrodiagnostic testing is to compare the speed of conduction in the median nerve with conduction in other nerves supplying the hand. When the median nerve is compressed, as in CTS, it will conduct more slowly than normal and more slowly than other nerves. There are many electrodiagnostic tests used to make a diagnosis of CTS, but the most sensitive, specific, and reliable test is the Combined Sensory Index (also known as Robinson index). Compression results in damage to the myelin sheath and manifests as delayed latencies and slowed conduction velocities . When pain is the primary symptom, carpal tunnel syndrome is unlikely to be the source of the symptoms. Nine flexor tendons and the median nerve pass through the carpal tunnel that is surrounded on three sides by the carpal bones that form an arch. The median nerve provides feeling or sensation to the thumb, index finger, long finger, and half of the ring finger. At the level of the wrist, the median nerve supplies the muscles at the base of the thumb that allow it to abduct, move away from the other four fingers, as well as move out of the plane of the palm. The carpal tunnel is located at the middle third of the base of the palm, bounded by the bony prominence of the scaphoid tubercle and trapezium at the base of the thumb, and the hamate hook that can be palpated along the axis of the ring finger. From the anatomical position, the carpal tunnel is bordered on the anterior surface by the transverse carpal ligament, also known as the flexor retinaculum. The flexor retinaculum is a strong, fibrous band that attaches to the pisiform and the hamulus of the hamate. The proximal boundary is the distal wrist skin crease, and the distal boundary is approximated by a line known as Kaplan's cardinal line. Simply flexing the wrist to 9. Compression of the median nerve as it runs deep to the transverse carpal ligament (TCL) causes atrophy of the thenar eminence, weakness of the flexor pollicis brevis, opponens pollicis, abductor pollicis brevis, as well as sensory loss in the digits supplied by the median nerve. The superficial sensory branch of the median nerve, which provides sensation to the base of the palm, branches proximal to the TCL and travels superficial to it. Thus, this branch spared in carpal tunnel syndrome, and there is no loss of palmar sensation. The potential role of B- vitamins in preventing or treating carpal tunnel syndrome has not been proven. Stretching before the activity and during breaks will aid in alleviating tension at the wrist. An example for an isometric exercise of the wrist is done by clenching the fist tightly, releasing and fanning out fingers. Early surgery with carpal tunnel release is indicated where there is evidence of median nerve denervation or a person elects to proceed directly to surgical treatment. In 1. 99. 3, The American Academy of Neurology recommend a non- invasive treatment for the CTS at the beginning (except for sensitive or motor deficit or grave report at EMG/ENG): a therapy using splints was indicated for light and moderate pathology. In general, local steroid injections are only used until other treatment options can be identified. Surgery. It is recommended when there is static (constant, not just intermittent) numbness, muscle weakness, or atrophy, and when night- splinting or other conservative interventions no longer control intermittent symptoms. However, surgery and wearing a brace resulted in similar symptom relief in the long term (1. Practitioners caution that any physiotherapy such as myofascial release may take weeks of persistent application to effectively manage carpal tunnel syndrome. For example, some have claimed that switching from a QWERTY computer keyboard layout to a more optimised ergonomic layout such as Dvorak was commonly cited as beneficial in early CTS studies, however some meta- analyses of these studies claim that the evidence that they present is limited. Two different techniques were used. The left scar is 6 weeks old, the right scar is 2 weeks old.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
December 2016
Categories |
 RSS Feed
RSS Feed
